New York City’s overall life expectancy has climbed back to near record levels after the steep declines of the COVID-19 pandemic, yet vast differences persist across racial, economic and geographic lines that reveal deep structural inequalities influencing how long residents live and how well they age.
According to the latest data from the New York City Health Department, average life expectancy for New Yorkers reached 82.6 years in 2023, matching pre-pandemic numbers and even recording a slight uptick in provisional 2024 figures. Preliminary reporting indicates the city may already have surpassed 83 years which was a goal set by public health officials for 2030, sooner than expected.
But behind these headline figures lie stark disparities. Black New Yorkers, for example, had a life expectancy of roughly 78.3 years, substantially lower than white residents at 83.3 years and Asian and Pacific Islander residents at 86.9 years. Latino New Yorkers fell between at about 82.8 years. These gaps reflect historic inequality in access to health care, exposure to stress and chronic conditions and social determinants of health that public health leaders link directly to structural racism and economic exclusion.
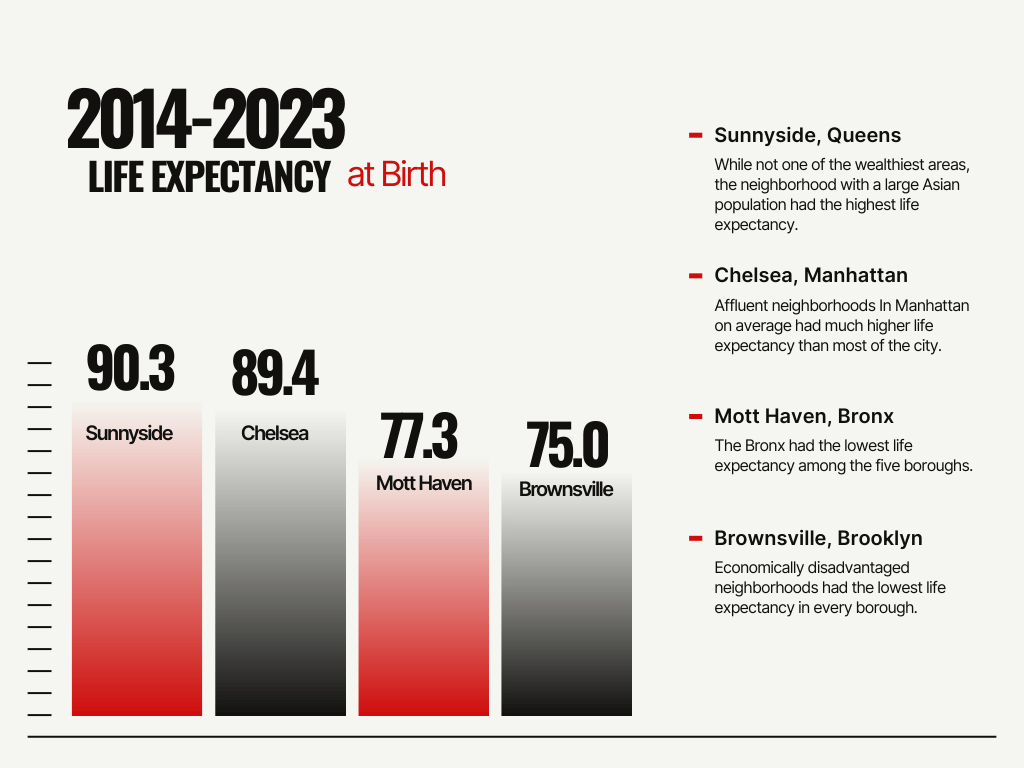
Neighborhoods tell a similarly uneven story. Data mapping tools show over a 15 year life expectancy gap between some communities, from a low of about 75 years in Brownsville, Brooklyn to a high of 90.3 years in of Sunnyside, Queens. These differences correlate strongly with income, housing quality, access to care and local environmental conditions.
Life expectancy is not just a number. It reflects how factors such as income inequality, affordable housing, access to health care, safety, diet, education and environmental conditions affect daily life. For many New Yorkers, these differences mean that a child born in one ZIP code may have a substantially shorter expected lifespan than one born a few miles away.
Racial inequity is perhaps the most visible dimension. The Black community’s lower life expectancy is linked to a number of factors identified in public health reporting, including higher rates of drug-related deaths and infant mortality that far exceed those of other groups. In 2023 the infant mortality rate for Black infants was nearly four times the rate for white infants.
Income plays an outsized role as well. Wealthier, majority white neighborhoods such as parts of Manhattan routinely report life expectancy well above the city average. In contrast, lower-income neighborhoods in the Bronx and Brooklyn, where median household incomes are significantly below city averages, have shorter lifespans. For example, in parts of the Bronx where median incomes are under $25,000, life expectancy often lags far behind wealthier areas.
Gender and social factors compound these disparities. Women in the city consistently live longer than men, a pattern that holds across racial and economic lines. Meanwhile, neighborhoods with higher concentrations of residents without easy access to primary care, fresh foods or safe open space see higher rates of chronic disease and premature death.
These inequalities have become a important policy issue for the city’s new mayor, Zohran Mamdani. During his campaign, Mamdani repeatedly highlighted structural inequities in housing, wages and access to care as drivers of poor health outcomes. He pledged that public health policy would be integrated with housing and economic policy, arguing that “New Yorkers cannot live healthier lives until they can afford housing, eat nutritious food and have safe spaces to exercise and breathe clean air.”
City officials have tied these health disparities to a broader policy agenda, including expanded community health programs, investments in preventive care and the creation of neighborhood health initiatives targeting the underlying social determinants of health.
Economic inequality also looms large. Life expectancy differences between the wealthiest and poorest neighborhoods reflect broader disparities in education, employment opportunities and housing stability. In some of the city’s lowest income neighborhoods, residents contend with the dual burden of limited access to preventive services and expensive health care. The mayor’s campaign rhetoric on affordable housing, rent stabilization and neighborhood investment will be tested as budget priorities are set this year.
Experts stress that lasting improvements in life expectancy cannot come from health care alone. “Health inequities are rooted in our economic and social systems,” said one public health researcher. Addressing them will require cross agency partnerships that integrate health, housing, education and labor policies which is an approach that Mamdani has advocated but has yet to fully implement.
Surpassing a citywide life expectancy goal years ahead of schedule may be progress, but the uneven distribution of those gains brings into sharp focus the unfinished work of closing the gap between the haves and have-nots. As Mayor Mamdani takes the reins, the test will not only be raising the overall average age of New Yorkers but ensuring that every community has a fair shot at a long, healthy life.



































































